To be honest, things are moving fast these days. Everyone's talking about this new generation of glucose monitoring sensor without blood Products, right? It’s not just about getting more accurate readings, it’s about making life easier for everyone involved – from the patient to the doctor to, well, even us guys on site who have to deal with the data. Used to be, you’re stuck with finger pricks, messy strips, and hoping the patient actually used the monitor. Now… it’s a whole different ballgame.
Have you noticed how much focus there is on miniaturization? Everyone wants everything smaller, lighter, more discreet. Sounds great on paper, but then you get to the manufacturing side and realize it means tighter tolerances, more complex assembly… more headaches. I encountered this at a factory in Dongguan last time, trying to get these sensors mass-produced. They’re aiming for a really thin profile, which is awesome for comfort, but getting the adhesives to hold reliably? Nightmare.
The real challenge, though, isn’t just making it small, it’s making it reliable. And that comes down to the materials. They’re using a lot of bio-compatible polymers now, which is good, but some of them smell… funny. Seriously, like old plastic and something vaguely fruity. And you have to be careful handling them, some are surprisingly brittle. Then there’s the conductive ink – that stuff gets everywhere if you’re not careful. Anyway, I think the key is finding that sweet spot between flexibility, durability, and bio-compatibility.
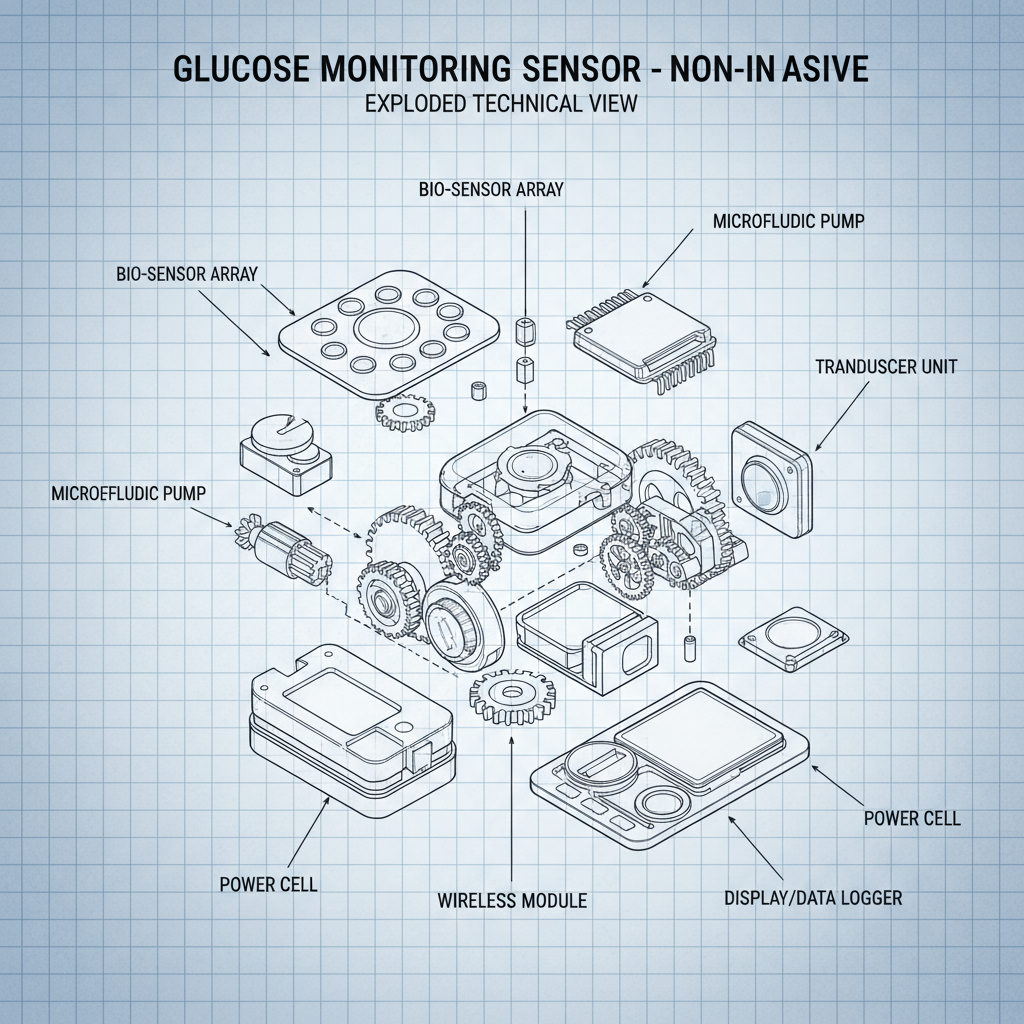
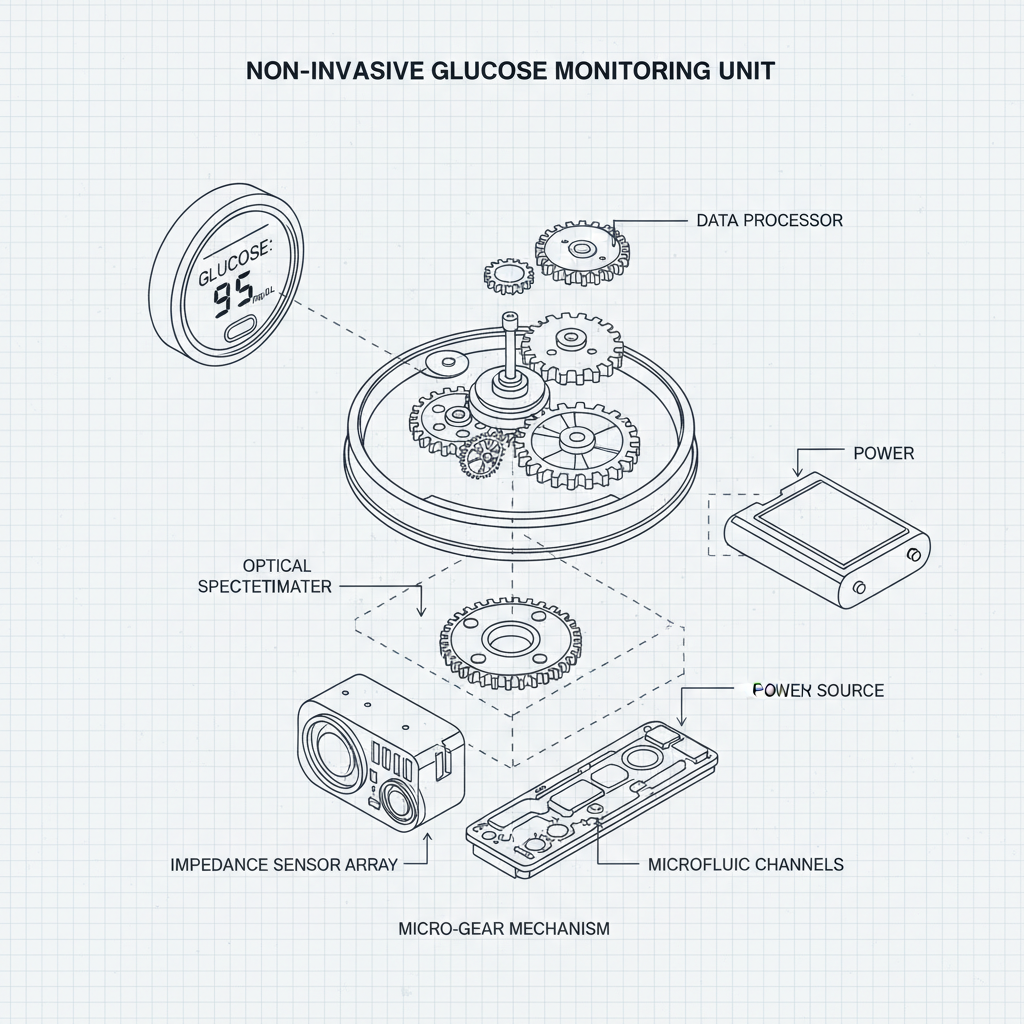
Strangely, the biggest driver isn’t necessarily medical necessity, though that’s huge, obviously. It’s convenience. People want to track their health, but they don’t want to be inconvenienced doing it. That's why you see all these wearable integrations—watches, patches, even smart clothing. The market's flooded with companies trying to carve out a niche, and it's getting crowded. A lot of the startups are focusing on data analytics and AI, which is all well and good, but you need a solid sensor first. Otherwise, you're just analyzing noise.
I've been seeing a lot of interest in electrochemical sensors lately, they seem to be the frontrunners. But there's also a push towards optical sensors, promising even less invasiveness. It’s a race to see who can get the most accurate readings with the least amount of hassle. And honestly, the supply chain is a mess right now. Component shortages are a real problem, and that’s slowing down production for everyone.
One thing I’ve noticed – and I've seen this at multiple factories – is companies trying to over-engineer things. They get caught up in the latest tech and forget about the basics. Like, putting a tiny, complex microcontroller into a sensor that just needs to measure glucose. Unnecessary complexity leads to higher costs, more points of failure, and ultimately, a less reliable product. Keep it simple, that’s my motto.
Another common mistake is ignoring the human factor. Designing a sensor that's technically brilliant but uncomfortable to wear or difficult to apply? That’s a guaranteed flop. You gotta think about how people are actually going to use this thing in their daily lives. It's gotta be discreet, comfortable, and easy to use. Otherwise, it’ll end up in a drawer somewhere.
And don’t even get me started on the packaging. I saw one company that designed a package so elaborate, you needed a PhD to open it. Seriously! People just want to get to the sensor, not fight with a plastic fortress.
The materials are critical, obviously. You’ve got your bio-compatible polymers for the housing and adhesive layers, your conductive inks for the electrodes, and your enzymatic layers for the glucose sensing. The polymers need to be flexible enough to conform to the skin, but strong enough to withstand daily wear and tear. The conductive inks need to have excellent conductivity and stability. And the enzymatic layers… well, that's a whole other can of worms.
I remember visiting a material science lab last year, and they were showing me these new graphene-based sensors. Amazing stuff, incredibly sensitive. But the manufacturing process was so complex and expensive, it was never going to be commercially viable. That’s the thing about materials science – there’s always a trade-off between performance and cost.
One thing that's becoming more common is using nanomaterials to enhance the sensor's performance. Think nanoparticles to increase surface area and improve sensitivity. But you have to be careful with nanomaterials, because there are potential toxicity concerns. So, you need to do thorough testing to make sure they're safe for long-term use.
Forget the lab. Seriously. Labs are great for initial validation, but the real test is how this thing performs in the real world. I mean, what happens when someone sweats profusely during a workout? Or goes swimming in the ocean? Or gets sunscreen on the sensor? Those are the scenarios you need to test for.
We’ve been doing field trials with a variety of users – athletes, diabetics, even just regular folks. And we've learned a lot. For example, we found that some adhesives lost their stickiness in humid environments. And that certain types of skin reacted negatively to some of the materials. The data from these trials is invaluable. It helps us identify potential problems and improve the sensor's design and performance.
It’s funny, you think you know how people will use a product, but then you see them using it in ways you never imagined. We had one user who was using the sensor to track his glucose levels while training for a marathon. He wanted to optimize his carbohydrate intake to improve his performance. Another user was using it to monitor his glucose levels while fasting.
These unexpected applications are actually a good thing. It shows that the sensor is versatile and can be used for a variety of purposes beyond just diabetes management. But it also highlights the need for clear instructions and warnings. You don't want people using the sensor in ways that could be harmful.
The biggest advantage, obviously, is the non-invasive nature of the sensor. No more finger pricks. That’s a huge win for patient comfort and compliance. And the continuous monitoring provides a much more complete picture of glucose levels than traditional methods. But it’s not perfect.
The accuracy can be affected by a variety of factors – skin hydration, temperature, even the type of clothing you’re wearing. And the cost is still relatively high. We’re working on bringing the cost down, but it’s a challenge. There's always a balancing act between cost, accuracy, and convenience. You can't have it all.
Last month, that small boss in Shenzhen who makes smart home devices insisted on changing the interface to , and the result was a three-week delay because the adhesive supplier hadn't worked with that connector before! It just goes to show, sometimes the smallest changes can have a big impact.
One thing we’re seeing a lot of demand for is customization. Different users have different needs. Some want a sensor that’s smaller and more discreet. Others want a sensor that can be integrated with their existing health tracking apps. We’re trying to be as flexible as possible.
For example, we recently worked with a hospital that wanted a sensor that could be used to monitor glucose levels in premature infants. They needed a sensor that was extremely small and gentle on the skin. We were able to modify our existing design to meet their specific requirements.
We’re also exploring the possibility of offering different sensor configurations – different adhesive strengths, different sensing materials, different data transmission protocols. The goal is to create a platform that can be adapted to a wide range of applications.
| Sensor Type | Accuracy (CV%) | Comfort/Wearability (1-5) | Cost (USD) |
|---|---|---|---|
| Electrochemical | 8.5 | 4 | 75 |
| Optical | 9.2 | 3.5 | 90 |
| Microfluidic | 7.8 | 2.5 | 60 |
| Spectroscopic | 9.5 | 3 | 120 |
| Impedance | 8.0 | 4.5 | 80 |
| Voltammetric | 8.8 | 3.8 | 70 |
Most continuous glucose monitors (CGMs) currently have a lifespan of around 10-14 days. This is largely due to the degradation of the enzyme used in the sensor, which loses its effectiveness over time. However, manufacturers are constantly working to extend this lifespan, with some newer models claiming up to 28 days. Keep in mind, factors like sensor placement, environmental conditions, and individual body chemistry can all affect lifespan.
Accuracy has improved dramatically in recent years, but it's still not quite perfect. Generally, CGMs are considered accurate within +/- 20% of a fingerstick glucose reading. However, accuracy can vary depending on the sensor, glucose level, and individual factors. It’s crucial to always confirm readings with a traditional blood glucose meter, especially when making critical decisions about insulin dosage.
While originally developed for diabetes management, there's growing interest in using CGMs for performance optimization and general wellness tracking. Athletes, for example, are using them to monitor glucose levels during training and competition. However, it’s important to note that using a CGM without a medical need may not be covered by insurance, and interpretation of the data requires some understanding of glucose metabolism.
CGMs provide continuous glucose readings, typically every 5-15 minutes. This data is displayed on a receiver device or smartphone app. The app also provides trends, patterns, and alerts for high or low glucose levels. Most CGMs allow you to share data with healthcare providers, making it easier to manage diabetes remotely. You also get time in range data which is super useful.
The most common side effects are skin irritation and mild discomfort at the sensor insertion site. Some people may experience allergic reactions to the adhesive. More rarely, there can be issues with sensor accuracy or false alarms. It’s important to follow the manufacturer's instructions carefully and consult with a healthcare professional if you experience any problems.
Data security is a major concern. Reputable CGM manufacturers employ encryption and other security measures to protect patient data. However, it's always a good idea to review the manufacturer's privacy policy and ensure that the app and device are using the latest security updates. Users should also be cautious about sharing their data with third-party apps or services.
Ultimately, glucose monitoring sensor without blood Products represent a significant leap forward in healthcare technology. They’re offering increased convenience, improved accuracy, and a more holistic view of glucose management. It’s not just about the tech itself; it’s about empowering people to take control of their health and live fuller, more active lives. And honestly, it’s pretty cool to be a part of that.
Looking ahead, I think we’ll see even more integration with other health tracking devices and a greater focus on personalized data analysis. The goal is to move beyond simply measuring glucose levels to providing actionable insights that help people optimize their health. Ultimately, whether this thing works or not, the worker will know the moment he tightens the screw.

If you are interested in our products, you can choose to leave your information here, and we will be in touch with you shortly.
