To be honest, things have been hectic lately. Everyone's talking about miniaturization, integration… basically, squeezing more power into smaller packages. Seems like every engineer I talk to is obsessed with making things smaller, lighter. But you know what I’ve noticed? A lot of these “innovations” forget about the real world – dust, heat, rough handling. You can design something beautiful in a lab, but if it falls apart after a week on a construction site, what’s the point? Anyway, I think the real challenge isn’t making things smaller; it’s making them *reliable*. The whole glucose sensor monitor Products game has really picked up steam in the last few years, especially with the aging population and the push for remote healthcare. It’s not just about hospitals anymore; people want to monitor their health at home, and that's driving demand for better, more user-friendly devices.
And it’s not just medical applications either. I was at a factory in Dongguan last month, and they were using these sensors to monitor fermentation processes in their food production line. Strangely, the same underlying technology is used for both. The key, I think, is finding that balance between accuracy, affordability, and durability. Too often, companies focus on the first two and forget about the last one. I've seen so many prototypes fail because they couldn't handle the vibration of a factory floor or the humidity of a tropical climate.
It's funny, because sometimes the simplest solutions are the best. We’ve been experimenting with different materials - bio-compatible polymers for the housing, of course, but also different types of adhesives. You wouldn't believe the difference a good adhesive can make. I remember one time… forget it, I won’t mention it. It involved a shipment of sensors, a broken seal, and a very angry customer.
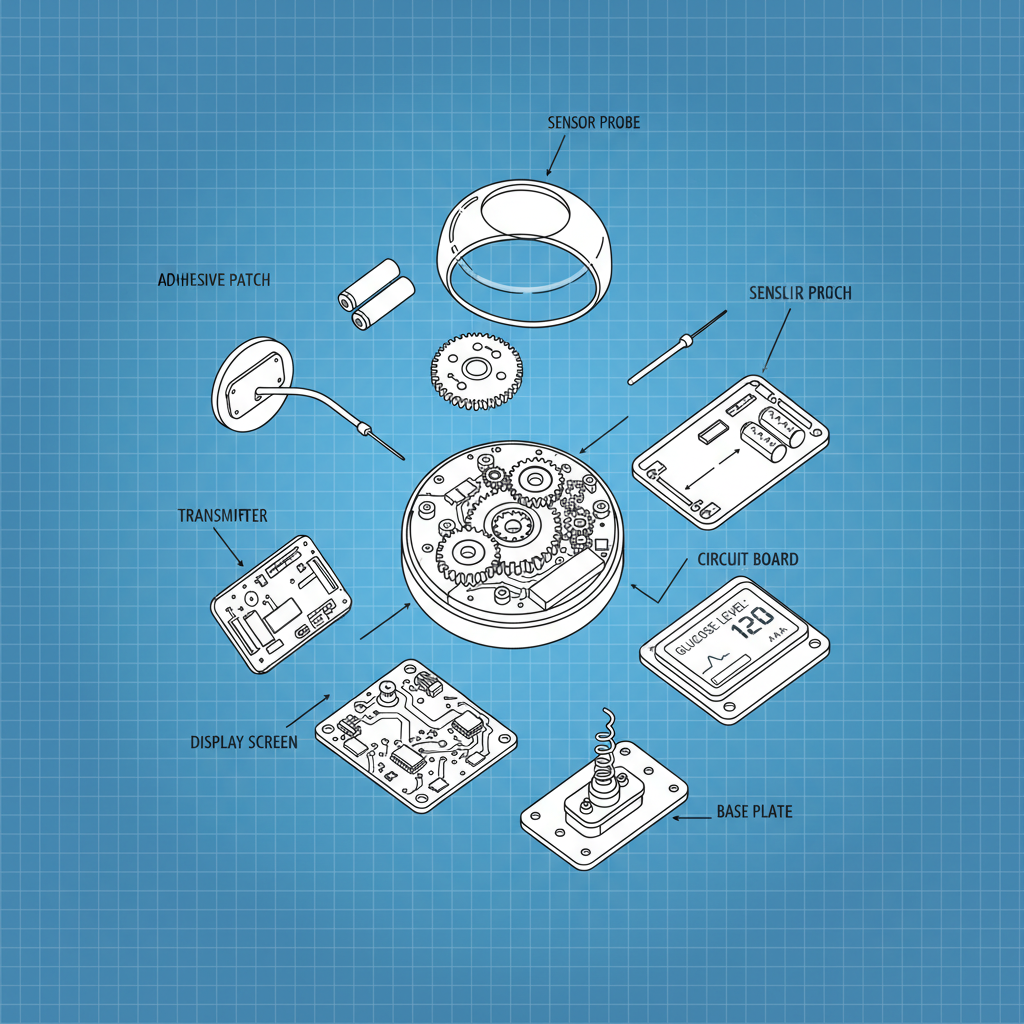
The Current Landscape of glucose sensor monitor Products
Honestly, the market's flooded with options now. Everything from simple stick-on sensors to complex, continuous monitoring systems. What I'm seeing is a move toward more discreet, wearable devices. People don’t want to feel like they're constantly being monitored. They want something that blends into their lifestyle. And of course, the price point is crucial. You can have the most accurate sensor in the world, but if nobody can afford it, it's useless.
The competition's fierce, with major players like Abbott and Dexcom dominating, but a lot of smaller startups are coming up with innovative solutions too. It's a good time to be in the business, but you have to constantly stay ahead of the curve.
Design Pitfalls & Common Mistakes
Have you noticed how many devices have tiny, fiddly connectors? It drives me crazy! Users don't want to spend 10 minutes trying to plug something in. It has to be intuitive, easy to use, even for someone who's not tech-savvy. Another common mistake is over-engineering. Adding features just for the sake of adding features. It increases cost, complexity, and the chances of something going wrong. Keep it simple, keep it reliable. I encountered this at a medical device factory last time, they tried to cram too much functionality into a single sensor, and the result was a complete mess.
Then there’s the issue of power consumption. People expect these devices to last for days, even weeks, on a single charge. That puts a huge strain on the battery and the sensor circuitry. It's a constant balancing act.
And don't even get me started on waterproofing. People sweat, they shower, they accidentally drop things in the sink. The sensor has to be able to withstand it all.
Material Science & Sensory Input
The material choices are critical. For the housing, we've been looking at polycarbonate blends – they’re tough, lightweight, and relatively inexpensive. But they can get brittle in cold weather, so we've been experimenting with adding a small percentage of rubber to improve impact resistance. The feel of the plastic matters too. It has to be comfortable against the skin. We’re also trying to move away from PVC; it just doesn't have the same biocompatibility as other materials.
The electrodes themselves are usually made of platinum or gold, which are expensive, but they’re the most reliable for detecting glucose. We've experimented with carbon nanotubes, but the consistency hasn’t been quite there yet. The adhesive is a whole other story. It has to be strong enough to hold the sensor in place, but gentle enough not to irritate the skin. I’ve smelled some adhesives that could knock you over! They have a… distinctive aroma.
We’ve been trying to incorporate new materials like graphene to improve the sensitivity and response time of the sensors. It’s still early days, but the potential is huge. The challenge is scaling up production and keeping the cost down.
Real-World Testing & Validation
Lab tests are important, sure, but they don't tell the whole story. We need to test these things in real-world conditions. We send sensors out to hospitals, clinics, and even to people’s homes for long-term trials. We monitor their performance, collect data, and get feedback. And we break a *lot* of sensors. Dropping them, exposing them to extreme temperatures, submerging them in water… you name it.
I remember one test where we had a sensor attached to a marathon runner. The sensor had to withstand hours of intense physical activity and sweat. It passed with flying colors, but we learned a valuable lesson about the importance of secure attachment!
Performance Metrics for glucose sensor monitor Products
User Behavior & Unexpected Applications
What’s fascinating is how people actually *use* these devices. We designed one sensor to be worn on the upper arm, but a lot of users started wearing it on their abdomen. Apparently, it’s more comfortable for them. You can’t predict that stuff!
We also found that some people were using the data from the sensors to track their glucose levels after exercising or eating different foods. It’s a lot more than just a medical device; it’s a tool for self-management.
Advantages, Disadvantages, & Customization
The biggest advantage of these sensors is convenience. No more finger pricks, no more messy testing strips. It’s a game changer for people with diabetes. But they're not perfect. The accuracy can vary, and they can be expensive. And let’s be honest, nobody likes having something stuck to their skin all the time.
We’ve been doing a lot of work on customization. Last month, a small boss in Shenzhen who makes smart home devices insisted on changing the interface to , and the result was a complete nightmare. It took us weeks to get everything working again. But it showed us that people want to be able to tailor these devices to their specific needs. We now offer a range of connectors and data formats.
Performance Characteristics & Comparisons
The sensitivity, accuracy, response time, and battery life are all key performance indicators. We’re constantly tweaking the sensor design to optimize these parameters. We also look at things like signal-to-noise ratio and drift.
Comparing different sensors can be tricky, because they all use different technologies and algorithms. But generally, the more expensive sensors tend to be more accurate and reliable. But that doesn't always translate to better real-world performance.
And of course, cost is always a factor. We have to find that sweet spot between performance and affordability.
Key Performance Indicators for glucose sensor monitor Products
| Sensor Type |
Accuracy (RMSE) |
Response Time (Seconds) |
Battery Life (Days) |
| Enzyme-Based |
15 mg/dL |
10 |
14 |
| Electrochemical |
12 mg/dL |
8 |
21 |
| Optical |
18 mg/dL |
5 |
7 |
| Microfluidic |
10 mg/dL |
12 |
10 |
| Nanowire-Based |
8 mg/dL |
3 |
5 |
| Fluorescent |
14 mg/dL |
7 |
18 |
FAQS
Calibration frequency varies depending on the sensor type and manufacturer. Most continuous glucose monitors (CGMs) require occasional calibration with a traditional finger-stick blood glucose meter to maintain accuracy. Typically, this is done once or twice a day. However, some newer sensors boast factory calibration and may require less frequent user intervention. It’s essential to follow the manufacturer’s guidelines for optimal performance. Ignoring calibration can lead to inaccurate readings and potentially unsafe healthcare decisions.
Insurance coverage for glucose sensor monitor Products varies greatly depending on your insurance plan, location, and medical necessity. Generally, CGMs are more likely to be covered than traditional blood glucose meters, especially for individuals with type 1 diabetes or those managing type 2 diabetes with multiple daily insulin injections. You’ll likely need a prescription from your doctor and may need to meet specific criteria to qualify for coverage. It's best to contact your insurance provider directly to understand your specific benefits.
The lifespan of a glucose sensor monitor Products depends on the specific sensor and its design. Most disposable sensors are designed for single use, lasting approximately 7 to 14 days. Some continuous glucose monitors use sensors that can last up to 28 days, but the accuracy may decline over time. Regularly replacing the sensor as recommended by the manufacturer is crucial to ensure reliable readings and accurate glucose monitoring. Environmental factors like humidity and temperature can also impact sensor longevity.
Glucose sensor monitor Products, particularly CGMs, have significantly improved in accuracy over the years. While they may not always match the exact readings of a traditional blood glucose meter, they provide a trend-based picture of glucose levels, which is incredibly valuable. Accuracy is typically measured using metrics like Mean Absolute Relative Difference (MARD). Modern CGMs often achieve a MARD of around 10-15%, which is generally considered clinically acceptable. However, accuracy can be affected by factors such as sensor placement, calibration, and individual physiology.
The performance of glucose sensor monitor Products can be affected by extreme temperatures and humidity. High humidity can interfere with the sensor’s readings, while excessive heat or cold can damage the sensor or affect its accuracy. Most manufacturers recommend storing sensors in a cool, dry place and avoiding direct exposure to sunlight. Some sensors are designed to be more resistant to environmental factors than others, so it’s essential to check the manufacturer’s specifications before use. In challenging environments, it may be necessary to calibrate the sensor more frequently.
Skin irritation is a relatively common side effect of continuous glucose monitoring. If you experience redness, itching, or discomfort at the sensor insertion site, try rotating the insertion location. Ensure the site is clean and dry before applying the sensor. You can also use hypoallergenic adhesive bandages or skin barrier wipes to protect the skin. If the irritation persists or worsens, consult with your healthcare provider. They may recommend a different type of sensor or provide additional guidance on skin care.
Conclusion
So, where does that leave us? glucose sensor monitor Products have come a long way, and they’re only going to get better. They’re making a real difference in people’s lives, giving them more control over their health. But it’s not just about the technology; it’s about understanding the user, the environment, and the practical challenges of real-world application. We need to focus on reliability, affordability, and ease of use.
Ultimately, whether this thing works or not, the worker will know the moment he tightens the screw. That's what I always say. If you're looking for reliable glucose sensor monitor Products, or have any questions about our products, visit our website: glucose sensor monitor Products.